Cholera and the Queen City
By: Megan Dunlevy
Cholera is a gastrointestinal disease caused by the bacteria Vibrio Cholerae. Cholera can be spread by consuming water than has been contaminated with the Vibrio Cholerae bacterium. Symptoms of cholera include diarrhea, vomiting and leg cramps and in severe cases, a rapid loss of fluids can result in dehydration or shock. Without treatment death can occur within a couple of hours after symptoms present. Contamination can be caused by poor sanitation, stagnant water, poor hygiene and little water treatment. Cholera cannot be spread from person to person so transmission from causal contact is not likely, but in dense population locations with poor sanitation, transmission can be rapid throughout an area.
Due to poor living conditions of the working class, lack of proper sanitation, and lack of clean drinking water, most urban areas saw recurrent cholera infections. The United States reached epidemic levels of cholera in 1832, 1849 and 1866 (Pyle). Cincinnati was not immune from these phenomena. By searching the digitized Cincinnati birth and death records, 422 Irish immigrants died from cholera between 1865 and 1912. For the purpose of this analysis, 365 records were used, as these records contained an address that could be mapped. Of the 365 records used, 162(44.4%) were men and 203( 55.6%) were women. Two hundred sixty-eight (73.4%) of the records are from the 1866 epidemic. It was not uncommon for cholera to be blamed on the Irish due to their religion (anti-Catholic sentiments blamed the disease on a vengeful God) or because of their poor living conditions (Daly). The actual infectious nature of cholera was unknown until the 1849 epidemic in London where it was shown by John Snow that cholera is transmitted in water sources (Pyle). The 1866 epidemic started in New York City where it was presumably brought over from Europe. From New York, the epidemic moved westward and south following the path of both the Ohio and Mississippi rivers and the new national railroad system (Pyle). The Civil War and interactions with Native Americans also contributed to the spread of cholera outside main waterways (Pyle).
Cincinnati had seen epidemic levels of cholera in 1832 and 1849 during which 4% of the city’s population died from cholera (Carter). Between the canal and steamboat traffic along the Ohio River, Cincinnati was in prime position to be affected by cholera contamination in waterways. Despite the 1832 and 1849 epidemics, Cincinnati did very little to improve the conditions that cause cholera. In fact when Dr. Daniel Drake tried to increase awareness of cholera during the 1832 epidemic, he was met with resistance and disbelief (Carter). For these reasons, Cincinnati failed to make the sanitation changes which other cities such as Pittsburgh and Charleston implemented that reduced the effect of future cholera outbreaks (Carter). The lack of sanitation changes and the clustering of the Irish in the poorest part of Cincinnati near the river made the Cincinnati Irish an easy target for the cholera epidemic.
Medical care for cholera was limited in the 1800s. As the mode of transmission was unclear, doctors had very little data to work with to treat their patients. Some cities fired a cannon in the middle of town to clear the air and lit fires at corners, but often during a cholera epidemic people fled the city for fear that the disease could be carried in the air (Daly). The flight of people also contributed to the spread of the disease. Often people with cholera would first show symptoms in the morning and be dead by the evening (Carter). Common treatments for cholera included bleeding, purging, opium and astringents (Daly). There was no means of an objective diagnosis as physicians did not know the cause (Daly). Until the 1900s and the improvements to sanitation and clean drinking water for urban environments, cholera would remain a part of life for poor urban Americans.
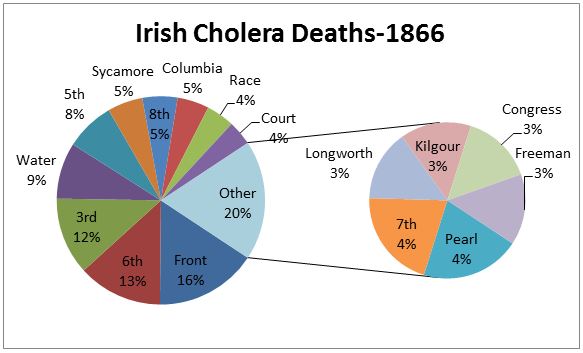
Nested pie chart showing the breakdown of addresses of the 1866 Irish cholera deaths (Only top 50% shown).
Cincinnati map from The Queen City in 1869 by George E. Stevens. Taken from University of Cincinnati Archives and Rare Books Library digital collection (https://www.libraries.uc.edu/arb/collections/urban-studies/cincinnati-maps.html)
References
Carter, Ruth C. “Cincinnatians and Cholera: Attitudes Towards the Epidemics of 1832 and 1849” Queen City Heritage. 32-48. http://bicetech.net/dbice/Schell/German%20Prodistent%20Orphanage/Cholera%20incinnati.pdf
“Cincinnati Birth and Death Records, 1865-1912.” 2017. University of Cincinnati Digital Resource Commons. University of Cincinnati Historical Records. http://digital.libraries.uc.edu/collections/birthdeath/
Centers for Disease Control and Prevention. Cholera- Vibrio Cholerae Infection. 9 November 2016. 27 March 2017 <https://www.cdc.gov/cholera/general/index.html>
Daly, Walter J. “The Black Cholera Comes to the Central Valley of America in the 19th Century – 1832, 1849, and Later.” Transactions of the American Clinical and Climatological Association 119 (2008): 143–153. Print.
Pyle, G. F. (1969).”The Diffusion of Cholera in the United States in the Nineteenth Century. Geographical Analysis” 1: 59–75. doi:10.1111/j.1538-4632.1969.tb00605.x